Bleak —
In polls, the unvaccinated are the least worried about the delta variant.
Beth Mole
–
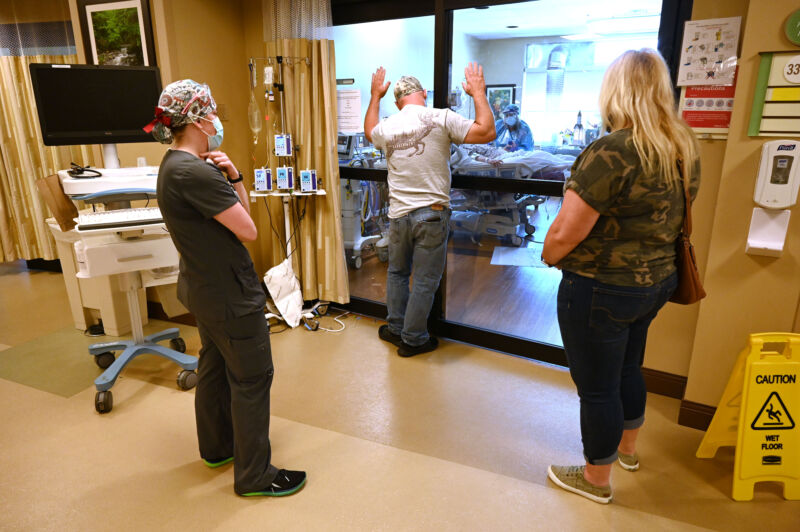
Enlarge / Anthony Church says goodbye through glass windows to his daughter, who is recovering from COVID-19 at Johnston Memorial Hospital’s ICU on June 16, 2021, in Abingdon, Va.
With the rapid rise of the highly transmissible delta variant and national vaccination efforts largely stalled, the COVID-19 pandemic continues to rage among the unvaccinated in the US—and things are looking grim.
Cases of COVID-19 are rising in all 50 states and the District of Columbia. Right now, the states with the highest averages for daily new cases per 100,000 people are Arkansas, Missouri, Florida, Louisiana, and Nevada, which all have below-average vaccination rates. Nationwide, average daily cases are up 140 percent over the past two weeks. Hospitalizations and deaths, which lag behind increases in cases by weeks, are also up 34 percent and 33 percent, respectively.
Relative to the rest of the pandemic, the nationwide numbers of cases, hospitalizations, and deaths are low—they’re matching or are below numbers seen back in April of 2020. But rates of cases among the unvaccinated in some places rival those seen at the heights of the pandemic. And areas with low vaccination coverage are seeing surges.
Missouri—with just 40 percent of its population fully vaccinated—is seeing daily new case rates as high as those seen last October, at the foot of the winter peak. And some hot spots in the state are setting records. In the southwestern county of Taney, for instance, the seven-day average for daily new cases is higher now than at any point previously, with an average of 55 new cases per day. The previous highest average was 45 new cases per day, which the county hit on November 22 and again on December 10. Across the border in Arkansas, Baxter county set a record last week for its highest average of daily new cases, which was 42 new cases per day. That surpassed its previous record of 32, set in early January. Only 33 percent of Baxter county’s population is fully vaccinated.
These case surges are translating to increases in hospitalizations. In Baxter, hospitalizations are up 340 percent over the last two weeks. In southwestern Missouri, hospitals have become overwhelmed, with intensive care units hitting capacity, ventilators running low, and hospitals reporting nursing shortages. Last week, Missouri’s Springfield-Greene County Health Department requested state funding to set up a field hospital to help handle the surge in patients with severe COVID-19 cases.
Vulnerabilities
In these places and elsewhere across the country, the vast majority of those hospitalized with COVID-19 are unvaccinated. In a White House press briefing last Friday, Rochelle Walensky, director of the Centers for Disease Control and Prevention, reiterated that more than 97 percent of COVID-19 patients entering hospitals nationwide are unvaccinated.
Along with the low vaccination rates, the spread of the delta coronavirus variant is behind the bleak surges. Delta is estimated to be more than twice as infectious as the original pandemic coronavirus strain. Since it was first detected in India in December 2020, it has become the most dominant variant in the world. And since it was first detected in the US in March, it has become the dominant strain here, quickly overtaking alpha (B.1.1.7). Helping the hyper-transmissible variant spread is the fact that it arrived just as many people in the US began letting their guard down, easing mask use and physical distancing.
Fully vaccinated people are largely protected from delta; the current vaccines are still highly effective against developing COVID-19 from delta and other variants of concern. Though a small proportion of people can develop so-called “breakthrough infections,” those infections will mostly be asymptomatic or mild. But unvaccinated people are completely vulnerable. Moreover, those who have received only one dose of a two-dose vaccine or have only recovered from COVID-19 are not much better off than those who are completely unvaccinated.
In a study published in Nature earlier this month, researchers tested the immune responses of people who had recovered from COVID-19 early on in the pandemic, before delta arose. Specifically, the researchers looked at the participants’ neutralizing antibodies—the most potent type of antibody that is thought to be critical for protection against the pandemic coronavirus. Looking at people who had recovered from early cases of COVID-19, researchers found their neutralizing antibodies were four- to six-fold less effective at fighting off the delta variant than they were at fighting off earlier versions of the virus. Likewise, people who had only received one dose of an mRNA vaccine barely had any detectable neutralizing antibodies that worked against delta.
But when recovered people received one vaccine dose or when partially vaccinated people received their second dose, neutralizing antibodies shot up, and both groups were considered highly protected.
Vaccination outlook
The finding spurred health experts to intensify their calls for vaccination, which is clearly effective against delta—if it’s done in time. Delta is spreading quickly, and it can take up to six weeks to become fully vaccinated and protected. It is critical for those who remain unvaccinated to get their shots as quickly as possible to avoid catching and spreading delta.
But according to new polling data from CBS News, a new wave of vaccinations seems unlikely. Among unvaccinated and partly vaccinated people, only 48 percent said they are concerned about delta. Among fully vaccinated people, 72 percent reported being concerned about the variant.
Despite the fact that the current COVID-19 vaccines have proven highly effective and safe, 53 percent of those who are unvaccinated or partly vaccinated said in the poll that they are concerned about side effects. Fifty percent of the group cited a lack of trust in the government as a reason not to get vaccinated. And 45 percent said they don’t trust the science. All of these percentages are higher than they have been in earlier polls, indicating that these anti-vaccine sentiments are hardening among the unvaccinated.
Some unvaccinated people who may be more persuadable have said they are waiting for the vaccines to receive full approval from the Food and Drug Administration (currently, they are authorized by the FDA under an emergency use authorization). On Friday, Pfizer and BioNTech said that the FDA had granted them a Priority Review designation for their mRNA vaccine, but they didn’t expect a decision on full approval until January 2022.
Currently, vaccine providers are administering only around 520,000 COVID-19 vaccines per day, down from a record of 4.6 million in a day in April. With over 161 million people vaccinated, only 48.6 percent of the US population is fully vaccinated.

